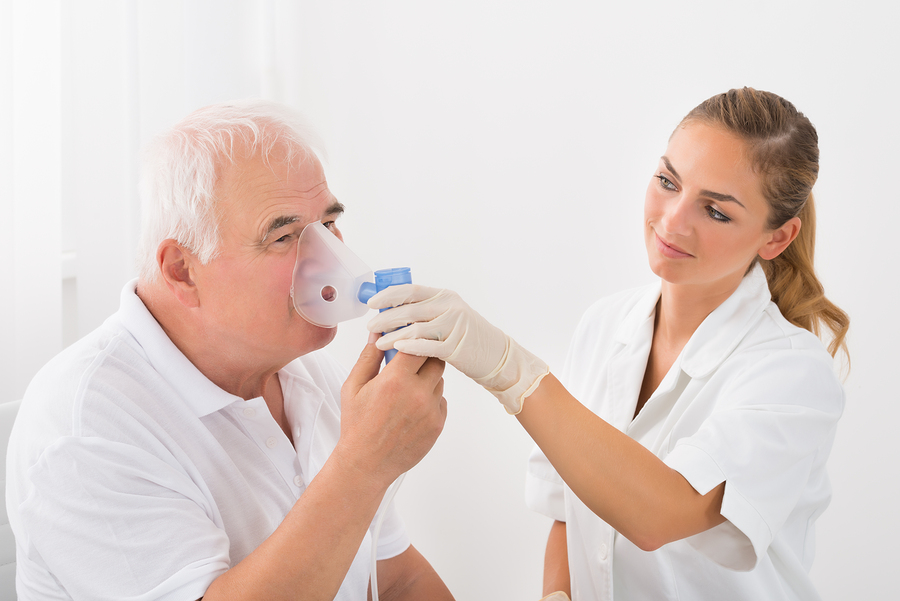
The Three Levels of Telehealth
Telemedicine is here, and the promise of empowered healthcare is becoming a reality. But there are significant differences in the levels of telehealth offered by providers. Understanding these differences is vital when implementing a long-term strategic plan for your patients and clients.
There are three fundamental levels of remote care. Each progressive level offers exponentially more services and capabilities for your targeted care population.
Level 1 – Remote Communication
We have had the ability to place a phone call for generations, and texting is the new norm. But more recently, healthcare has incorporated HIPAA-compliant video conferencing as a remote communication option.
Why is video so important?
Patients often have a hard time describing an issue – “I have swelling on my face,” or “my lips are cold and turning purple,” for example. Traditionally, a rural patient who would describe these to their provider over the phone might be advised to drive an hour or more into the hospital, so the care team can take a look. This has always been inconvenient, expensive, and potentially life-threatening, if a timely diagnosis and resulting action was required.
With a phone or tablet camera, the patient can now show their face – the swelling will easily be distinguished between mild or severe. The patient can show their oxygen tank and the care professional can see if the oxygen tank is either empty or turned off, resulting in cold, purple lips. Merely turning it back on or replacing the tank will save the hour drive and expensive hospital visit. It will also provide better and more timely care than a mere call or text can provide.
Level 2 – Remote Patient Monitoring
What distinguishes Remote Patient Monitoring (RPM) from remote patient communication is the ability to collect and pass biometric data real-time. The at-home patient has or is provided Bluetooth medical devices –– blood pressure cuffs, scales or pulse oximeters, etc., even a FitBit-type of activity tracker –– and the data from these devices can be passed instantaneously to the care team.
True RPM involves a care team available 24/7. An at-home or remote patient or client can transmit biometric data anytime. The care team reviews the data and provides guidance, monitoring for abnormal readings, or requests for a second or more frequent reading; all to monitor a patient’s health.
With RPM, medical professionals get most of the same data they would acquire with an inpatient visit, enabling them to make informed care decisions. Often, decisions help prevent the need for readmissions and the requirement to provide rooms and staff.
With these capabilities, RPM is a significant advancement over remote patient communication.
Level 3 – Remote Patient Engagement
But there is yet another level of RPM that provides much more for both the care team and patient, all while requiring no additional staff or facilities. Remote Patient Engagement (RPE) has been referred to as the difference between a calculator (remote patient communication), the first desktop computer (RPM), and the latest smart devices with 10 processors, terabytes of memory, and built-in, Siri-like capabilities (RPE).
True patient engagement incorporates predictive, proactive and preventative care. How does it do it?
Remote Patient Engagement platforms are the way of the future. Some RPE components:
- Surveys. Based on responses, the software can identify and predict potential upcoming issues.
- Medication Management. This feature reminds the patient to take medicine, provides proactive alerts if medicine is not taken, provides information about when and how to take medicine, and can be proactive when new medications are added.
- Nutrition Management. This feature, which can be voice-driven, records food intake and counts calories and nutritional information. It can provide recommendations and guidance for food intake, warn of excessive cholesterol, sugar, or other ingredients, and offer tutorials on food preparation.
- Tailored Education and Resource Library. Based on the medical issue of the patient, RPE not only provides a resource library, it can create a learning regimen for the patient and their family to become better educated on their specific condition. And it can all be accessed on the patient’s tablet or smart device.
- Secure Messaging. HIPAA-compliant communication is key for any remote healthcare solution. With RPE, texts, pictures and videos can be securely sent to the patient’s care team.
- Reward/Gamification. For true adoption of technology, rewards and gamification have proven to solidify use and loyalty. Advanced RPE platforms have built-in rewards and user-activated gamification for achieving goals, recording vitals, completing a task, reviewing education material and more. Healthcare providers can create and implement incentives and rewards to encourage adoption. This can also lower care costs over time.
- Family Participation. True RPE includes the active participation of close family members and friends. At the patient’s discretion, some or all of their data can be shared with family members and friends, who can then access the mobile app to help monitor the patient’s behavior and remind the patient of upcoming appointments and scheduled activities. They can also be on the patient’s list of those to be contacted by care providers for updates or concerns. Including friends and family in a patient’s care has proven to create better long-term outcomes.
- Smart Device Capable. True RPE includes all of the capabilities of Remote Patient Monitoring, including Bluetooth device integration, as well as monitoring of Activity Trackers. As more advanced devices are created, they will be seamlessly incorporated into the smart device network.
Do All Remote Patient Engagement Providers Offer All of These Capabilities?
The number of Remote Patient Engagement providers is understandably fewer than Remote Patient Monitoring. And within that subset, not all platforms offer all the services noted above. m.Care, developed by LifeScience Technologies, is one such platform that provides a full suite of capabilities.
m.Care technology burst on the scene in 2014 when it was competitively selected to provide the software to power Mercy Virtual, the first virtual healthcare center in the world. LifeScience Technologies’ history of utilizing technology to create modern healthcare solutions led to the development of a robust, highly configurable platform, to monitor all types of patient conditions and disease-states.
Their experience at building custom solutions proved critical in creating the interactive, highly successful PRE platform they provide today. While the platform is widely used for chronic care patient populations, it also has significant penetration in the mental and behavioral health space, corporate wellness, concierge medicine, and payer models.
Other Recent Articles
m.Care Technology – Predictive Capability, Interoperability, Ease of Integration, and Security

PRESS RELEASE: m.Care Virtual Care Platform Launches COVID-19 Long-Haulers Patient Monitoring

COVID Long-Haulers – Do You Have a Care Solution For This Patient Population?